Diabetic Retinopathy
What is diabetic retinopathy?
Diabetic Retinopathy results from deterioration of the retinal blood vessels. Over time, irregular levels of blood glucose damage small vessels in the body of a diabetic. Small vessels occur in the heart, kidney, peripheral circulation, and the retina of the eye. Damage to these retinal vessels diminishes the oxygen and nutrition available to the retina. Furthermore, the defective blood vessels leak and deposits of blood, lipid and fluid bog down the neural function of the retina as well. The retina acts like the film in the camera of the eye. If the film is bad, the picture is bad. Unfortunately, the retina cannot be replaced and any damage results in permanent vision loss.
There are two types of diabetic retinopathy: non-proliferative diabetic retinopathy (NPDR) and proliferative diabetic retinopathy (PDR).
-
NPDR is an early stage of diabetic retinopathy. NPDR occurs when the blood vessels in the retina leak which causes the retina to swell. NPDR initially does not affect vision unless edema is present in the macula, which is the area of retina responsible for central vision. As NPDR progresses, the retinal vessels can collapse and become obliterated; ischemia(lack of oxygen) results. If the ischemia is in the macula area, vision loss would be devastating and permanent.
-
PDR is a more advanced stage of diabetic retinopathy occurring after retinal vessel damage and collapse in the peripheral retina. When peripheral vessels are obliterated, new vessels begin developing on the retina in response to the ischemia. Unfortunately, these new vessels are abnormal, hemorrhage easily, and form scar tissue bands that detach and further damage the retina. PDR can result in more severe vision loss, including complete blindness.
The best treatment of diabetic retinopathy is prevention. If detected early, changes in the retinal blood vessels can be treated before vision loss occurs. Finally, meticulous control of the disease of diabetes itself goes a long way in maintaining good vision.





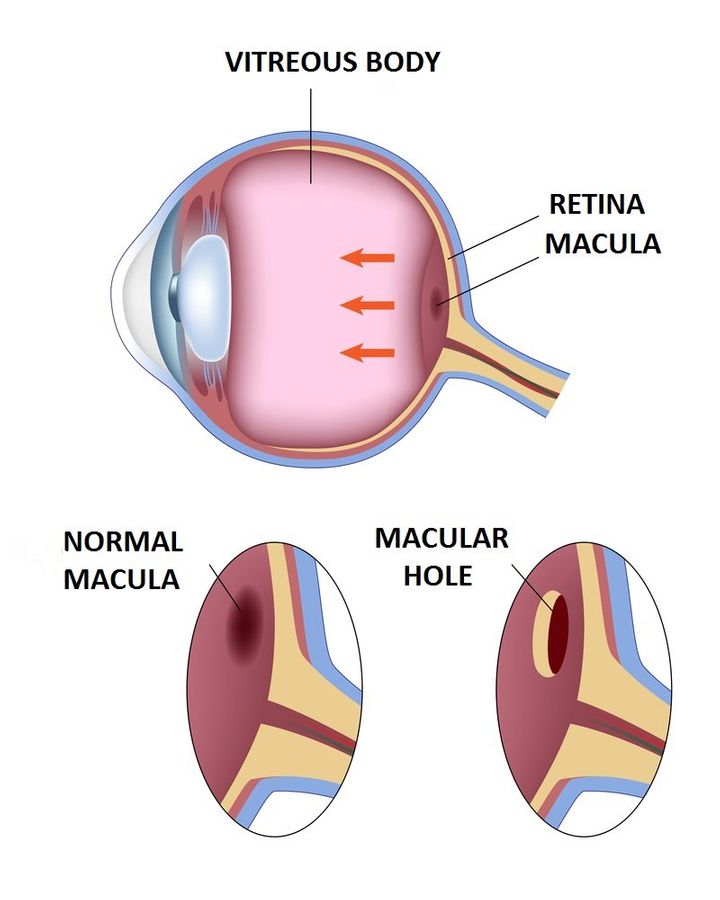 Macular Holes occur sporadically as a result of the natural aging process of the eye. The vitreous is the clear fluid inside the back of the eye and will shrink with age. The vitreous normally separates from the retina with no negative effect during this process. For some individuals, the vitreous does not separate seamlessly and instead continues to stick to the retina. If the vitreous remains attached to the central portion of the retina, called the macula, vision may be affected. The macular tissue will be stretched and can tear creating a macular hole. A surgical macular repair is the most effective way to treat a macular hole.
Macular Holes occur sporadically as a result of the natural aging process of the eye. The vitreous is the clear fluid inside the back of the eye and will shrink with age. The vitreous normally separates from the retina with no negative effect during this process. For some individuals, the vitreous does not separate seamlessly and instead continues to stick to the retina. If the vitreous remains attached to the central portion of the retina, called the macula, vision may be affected. The macular tissue will be stretched and can tear creating a macular hole. A surgical macular repair is the most effective way to treat a macular hole.